The answer is usually not about brushing harder or softer—it's about understanding how cold sensitivity differs from gum tenderness and what is actually triggering your gum sensitivity, which more often than not stems from the tools you are using every single day.
According to the CDC, nearly 42% of adults aged 30 and older have some form of periodontal disease. Sensitive gums are widespread, not a personal failure. Many of the most common causes are fixable once you know what to look for.
Key Takeaways
-
Gum sensitivity is most often caused by everyday habits and tools, especially brushing too hard or using a toothbrush without a true Sensitive mode
-
Hormonal changes, diabetes, stress, and nutritional deficiencies can amplify gum sensitivity by increasing inflammation and altering your gums' response to plaque
-
Proper oral hygiene with gentle brushing, correct flossing technique, and the right toothbrush can prevent and soothe sensitive gums
-
Persistent or worsening gum sensitivity, especially with bleeding, swelling, or loose teeth, requires prompt dental evaluation to prevent progression to gum disease
What Counts as Sensitive Gums? (Symptoms to Notice)
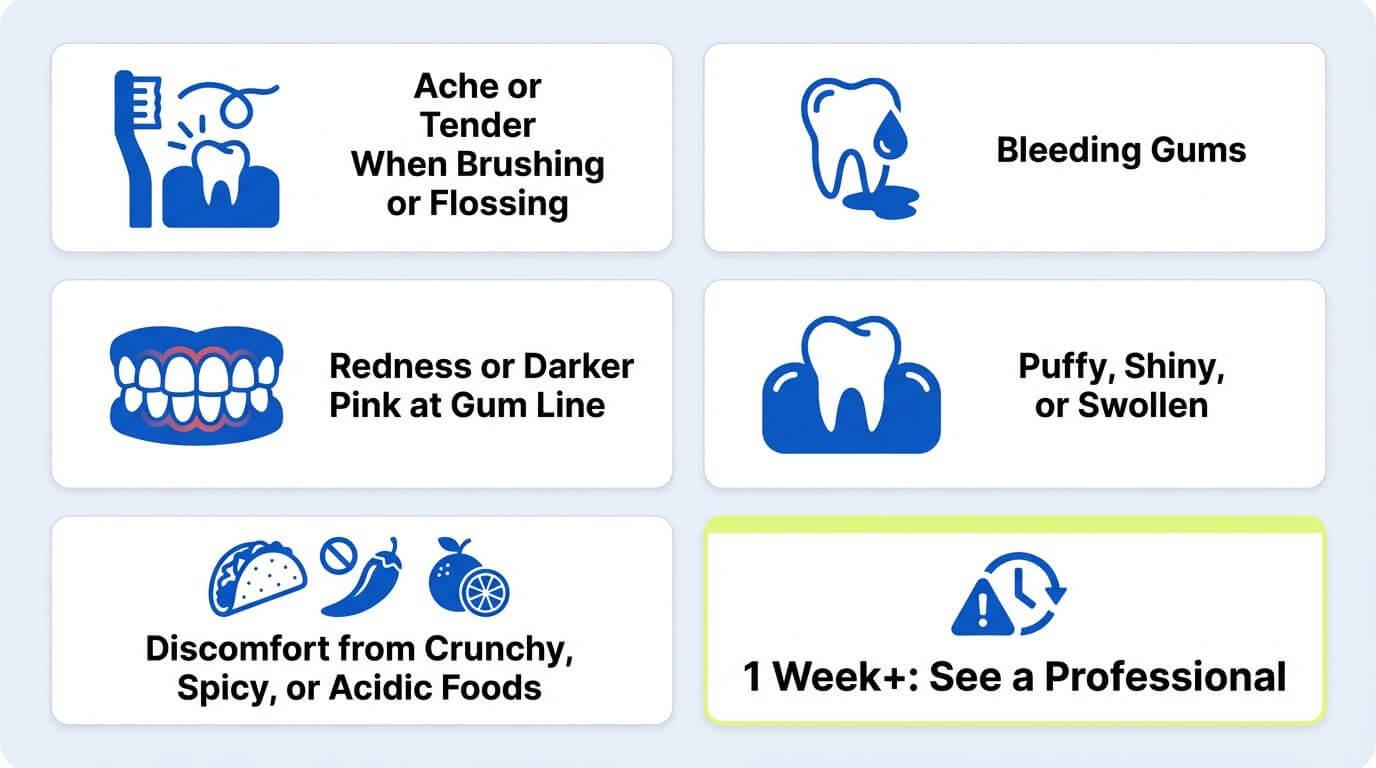
Gum sensitivity shows up as tenderness, soreness, or pain specifically in your gum tissue during brushing, flossing, or eating. It can be mild and brief after a dental cleaning, or it can linger for days without an obvious cause. We want you to know the difference so you can act on it.
Watch for these symptoms:
-
Gums that ache or feel tender when you brush or floss
-
Bleeding gums during brushing and flossing
-
Redness or a darker pink color along the gum line
-
Gums that look puffy, shiny, or slightly swollen
-
Discomfort when eating crunchy, spicy, or acidic foods
A quick distinction worth knowing: if ice water sends a sharp zing through a single specific tooth, that is likely tooth sensitivity from exposed dentin. If brushing makes a whole area of gum feel sore or tender, that is gum sensitivity. There are different issues that require different solutions.
If your symptoms persist beyond 1 week or are getting worse, that is your signal to get a professional exam rather than just applying more home care.
Most Common Everyday Causes of Sensitive Gums
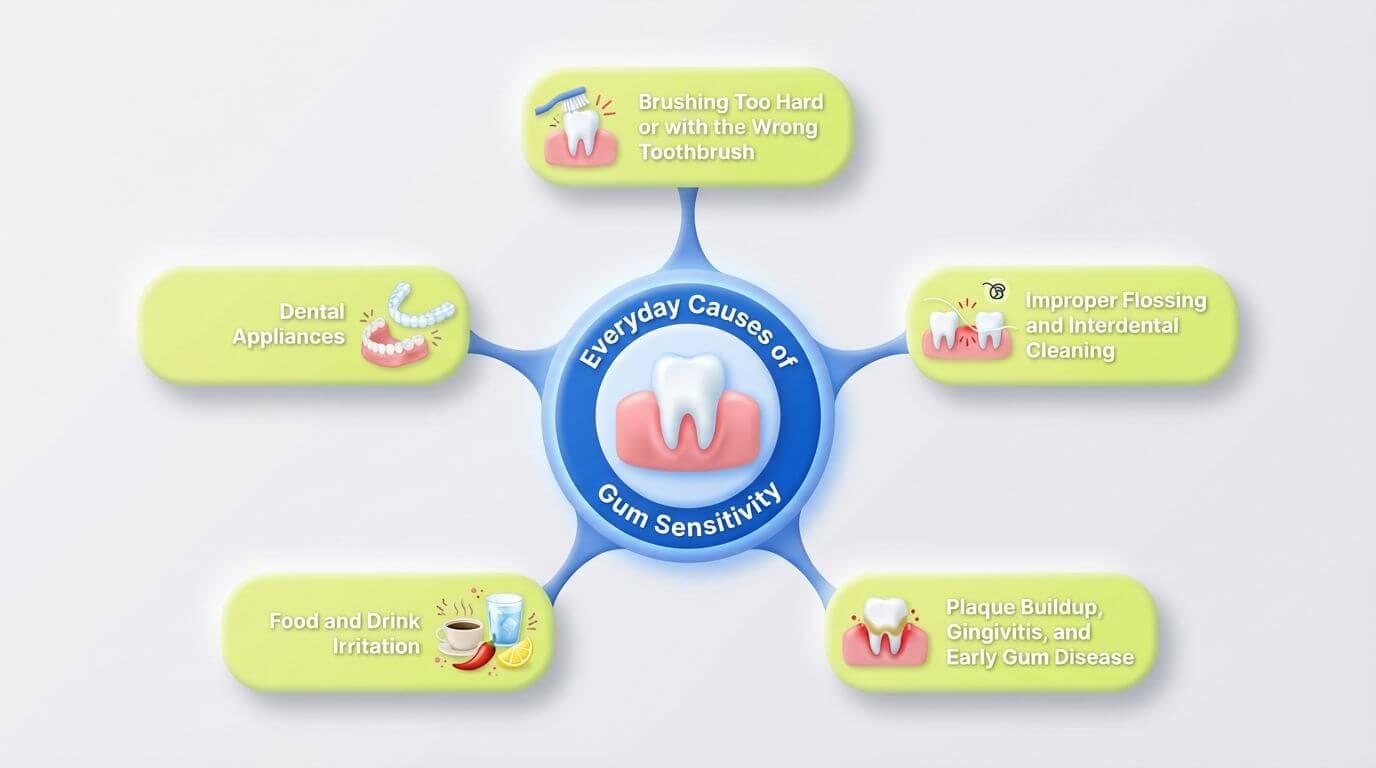
Most gum sensitivity comes from everyday habits and tools, not sudden infections or mystery diseases. Let us walk through the biggest culprits.
Brushing Too Hard or with the Wrong Toothbrush
Aggressive scrubbing and stiff bristles physically scrape your gum tissue, creating micro-abrasions, recession, and ongoing soreness. Most people brush harder than they realize.
A study published in the Journal of Periodontology found that subjects with a history of hard-brush use had nearly twice the rate of gum recession compared to those without. A 2025 narrative review in PMC confirmed that brushing forces above 3 N are directly associated with more severe gum recession and enamel loss.
Here is what happens with improper brushing:
-
Hard nylon bristles (0.15 to 0.20mm diameter) do not flex. They abrade.
-
Scrubbing motions traumatize gum tissue instead of cleaning it
-
Enamel and gum abrasion become long-term risks with repeated overbrushing
-
Frayed bristles signal wear that continues to cause damage with every use
-
Gums may appear notched or receded at the gum line over time
The label "soft" on the package is not always soft enough when combined with high motor intensity. An uncalibrated electric brush can apply uniform high-frequency vibrations without adapting to your gums' needs.
Improper Flossing and Interdental Cleaning
Snapping floss straight down into your gums or forcing oversized interdental brushes can cut or bruise the tissue, triggering gum soreness that people often mistake for gum disease.
If you are starting to floss after a long gap, expect some soreness for a few days. It should gradually improve, not worsen. Blood on your floss is not normal. It is a common early sign of gingivitis and a reason to improve your technique, not stop cleaning.
Plaque Buildup, Gingivitis, and Early Gum Disease
Plaque is a sticky biofilm of bacteria that forms within hours of eating. When it accumulates along your gum line, it irritates the tissue and triggers inflammation. Gingivitis is the first, reversible stage of gum disease: red, puffy, tender gums that may bleed when you brush or floss.
The tricky part: Gingivitis often doesn't hurt much, which is why people often dismiss bleeding as normal. But bleeding gums are an early warning, not something to ignore. Look for:
-
A reddish rim at the gum line
-
Bad breath that will not go away despite good brushing and flossing
-
Gums that look slightly swollen or shiny
Gingivitis can be reversed with improved brushing and flossing plus professional scaling. Left untreated, it progresses to periodontitis, which involves irreversible bone and attachment loss. The American Academy of Periodontology identifies scaling and root planing as the standard first-line treatment for periodontitis once gingivitis has progressed.
Food and Drink Irritation (Acidic, Sugary, and Spicy)
Acidic drinks and sugary snacks shift your mouth's pH, feeding bacteria and irritating already sensitive gum tissue. Common culprits include cola, energy drinks, sports drinks, bottled lemonade and citrus juices, sour candies, and vinegar-heavy dressings.
Simple habit shifts that help: rinse with plain water after acidic foods, avoid constant sipping throughout the day, and wait 30 to 60 minutes before brushing after consuming strong acids to avoid abrading softened enamel.
Dental Appliances (Braces, Aligners, Dentures, Mouthguards)
New dental appliances can rub or press on your gums, creating sore spots. This includes braces, clear aligners, retainers, night guards, and dentures. Normal adaptation soreness lasts for the first few days to weeks. But ongoing sharp or cutting pain is a signal that the appliance needs professional adjustment. Signs to watch for:
-
Metal brackets rubbing the inside of your lip or gum
-
A denture edge leaves a red groove in the gum tissue
-
An aligner tray pinching the gum margin
Dental wax for braces, professional adjustment, or denture relining can all resolve this. Do not push through it if your gums are breaking or ulcerated. Untreated sores can lead to oral infections.
When It's More Than Brushing: Medical and Lifestyle Causes
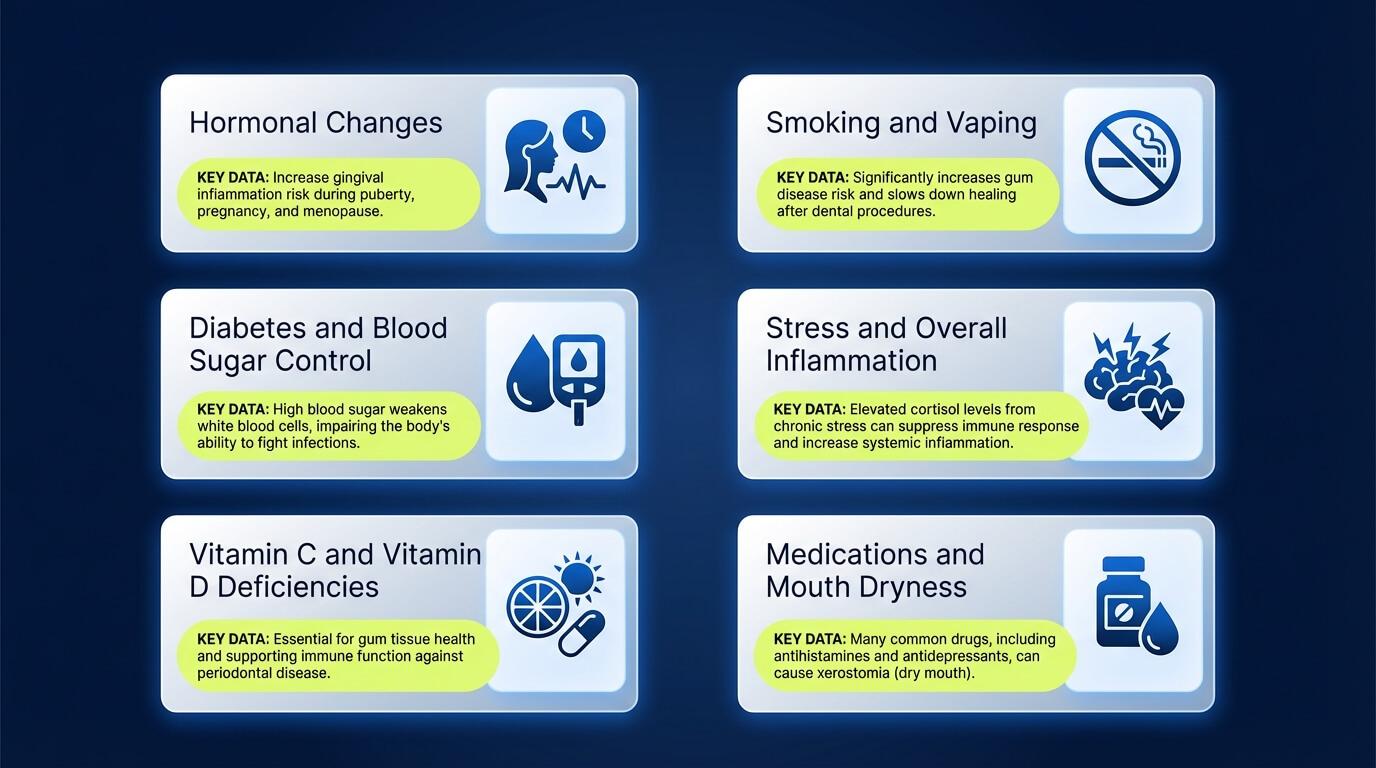
Sometimes, even with careful brushing and a consistent routine, gums remain sensitive because of what is happening in the rest of your body.
Hormones, immune changes, nutrient levels, stress, and medications can all make gums more prone to swelling and pain in response to the same amount of plaque.
Hormonal Changes Across Life Stages
Higher estrogen and progesterone levels increase blood flow to the gums and intensify their response to plaque. A systematic review published in PMC confirmed that gingival inflammation increases significantly throughout pregnancy and is greater in pregnant versus non-pregnant women, even without a corresponding increase in plaque levels. Hormonal changes affect multiple life stages:
-
Puberty: Teenagers notice bleeding gums for the first time as hormone levels surge
-
Menstrual cycle: Tender gums just before your period, known as menstrual gingivitis
-
Pregnancy: Pregnancy gingivitis affects 60 to 75% of pregnancies, causing increased bleeding and swollen gums (source)
-
Perimenopause and menopause: Dry mouth combined with tender, irritated gums that feel more reactive than before
Hormones alone do not cause gum disease. They amplify the gums' response to existing plaque or rough brushing. The same habits that caused no problem before can suddenly produce new soreness when hormone levels shift.
Diabetes and Blood Sugar Control
The connection is direct: higher blood sugar means more sugar in saliva, which feeds bacteria, increases plaque, and worsens gum inflammation. A review published in Diagnostics confirmed the bidirectional relationship between diabetes and periodontal disease. Diabetes increases the risk and severity of periodontitis, and in turn, gum disease can make blood sugar harder to control, creating a cycle that worsens both conditions.
If you have diabetes and notice gum pain persists, mention it at both your dental and medical appointments. Managing one condition actively supports the other.
Vitamin C and Vitamin D Deficiencies
A PMC review on vitamin C and oral health found that vitamin C deficiency can cause gingival bleeding regardless of oral hygiene and that individuals with lower blood levels of vitamin C exhibit more severe periodontal disease. Vitamin C is essential for collagen synthesis, which makes up the connective tissue that holds your gums in place.
A narrative review on vitamin C and D in periodontitis also confirmed that low vitamin D levels decrease gum immunity and increase inflammation, and that vitamin D concentration is inversely related to periodontitis severity.
If you experience persistent gum issues alongside fatigue, aches, or skin bruising, a medical checkup and blood tests may be warranted. Good sources of vitamin C include oranges, strawberries, and bell peppers. Good sources of vitamin D include fatty fish, fortified milk, and safe sun exposure.
Smoking and Vaping
Nicotine and other chemicals reduce blood flow to the gums, damage immune cells, and mask early warning signs such as bleeding. A systematic review and meta-analysis in PMC found that smoking raises the incidence of periodontitis by 85%.
The CDC confirms that tobacco use in any form, including cigarettes, pipes, and smokeless tobacco, raises your risk for gum disease and makes it harder for gums to heal after treatment.
The especially dangerous part: smoking can mask early warning signs. Your gums can be diseased without obvious bleeding or swelling until the damage is already advanced. If you smoke and have sensitive gums, see a dentist sooner rather than later.
Stress and Overall Inflammation
Chronic stress raises cortisol, the stress hormone, which increases inflammation throughout your body, including your gums. High stress can also indirectly worsen gum health by reducing attention to proper oral hygiene, increasing comfort snacking on sugary foods, and contributing to teeth grinding that traumatizes gum tissue. People under prolonged stress often report sore, easily bleeding gums, even when their routine has not changed.
Medications and Mouth Dryness
Many common medications, including antidepressants, some heart medicines, and antihistamines, cause dry mouth or gum overgrowth as side effects. Dry mouth reduces saliva, your mouth's natural cleanser, leading to increased plaque buildup and gum irritation. Do not stop any medication on your own. Talk to both your dentist and physician. Dentists can suggest saliva substitutes, fluoride toothpaste, or more frequent cleanings to manage the side effects.
Is This Gum Sensitivity or Something More Serious?
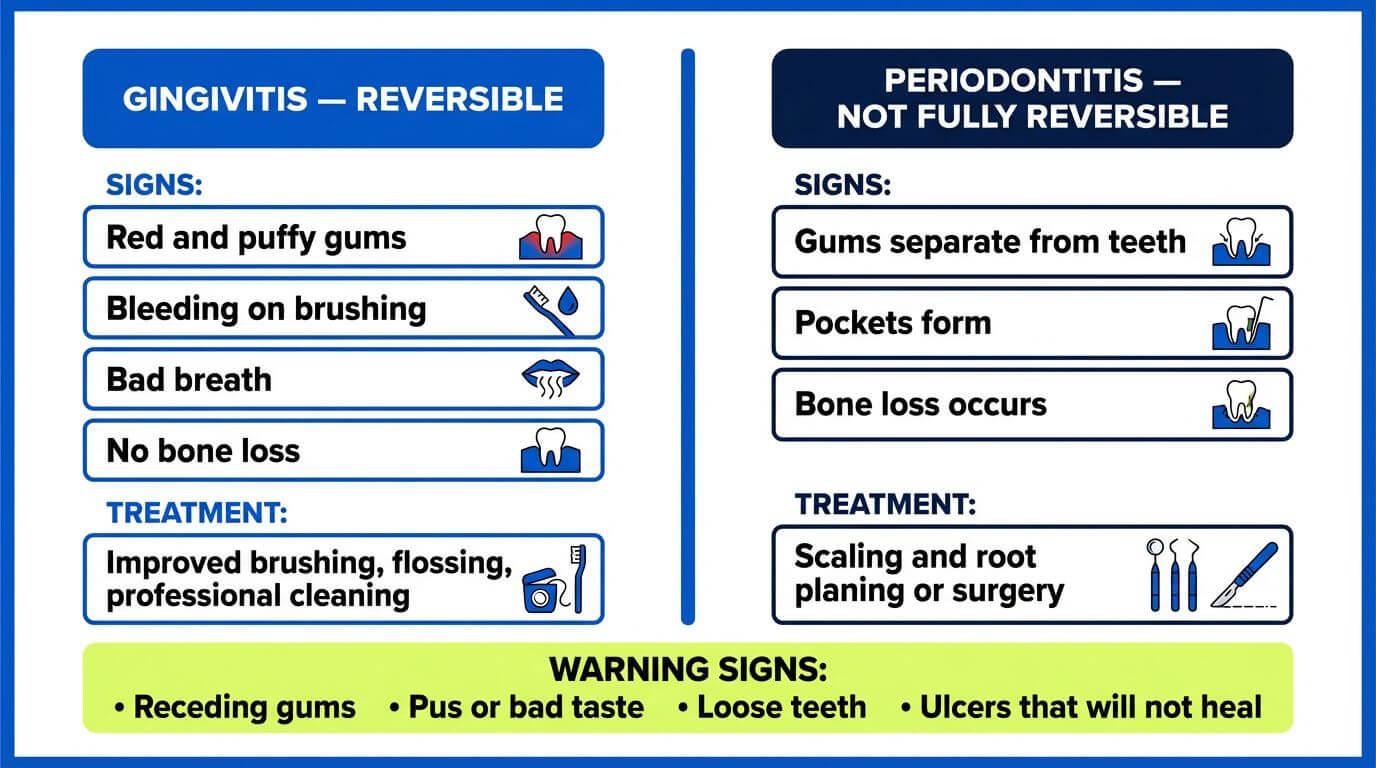
Mild gum soreness after a deep cleaning or when starting a new routine is common and resolves quickly. But certain patterns point to developing gum disease that needs professional attention.
Warning signs that require prompt dental care:
-
Receding gums or visible tooth root exposure
-
Pus, a bad taste, or persistent bad breath
-
Loose teeth or a changing bite
-
Canker sores or mouth ulcers that will not heal
Bleeding gums occur as an early warning, not a late one. Do not dismiss it as normal. Early intervention can often reverse gingivitis completely and prevent bone loss.
How Your Toothbrush Could Be Making Your Gums Sensitive
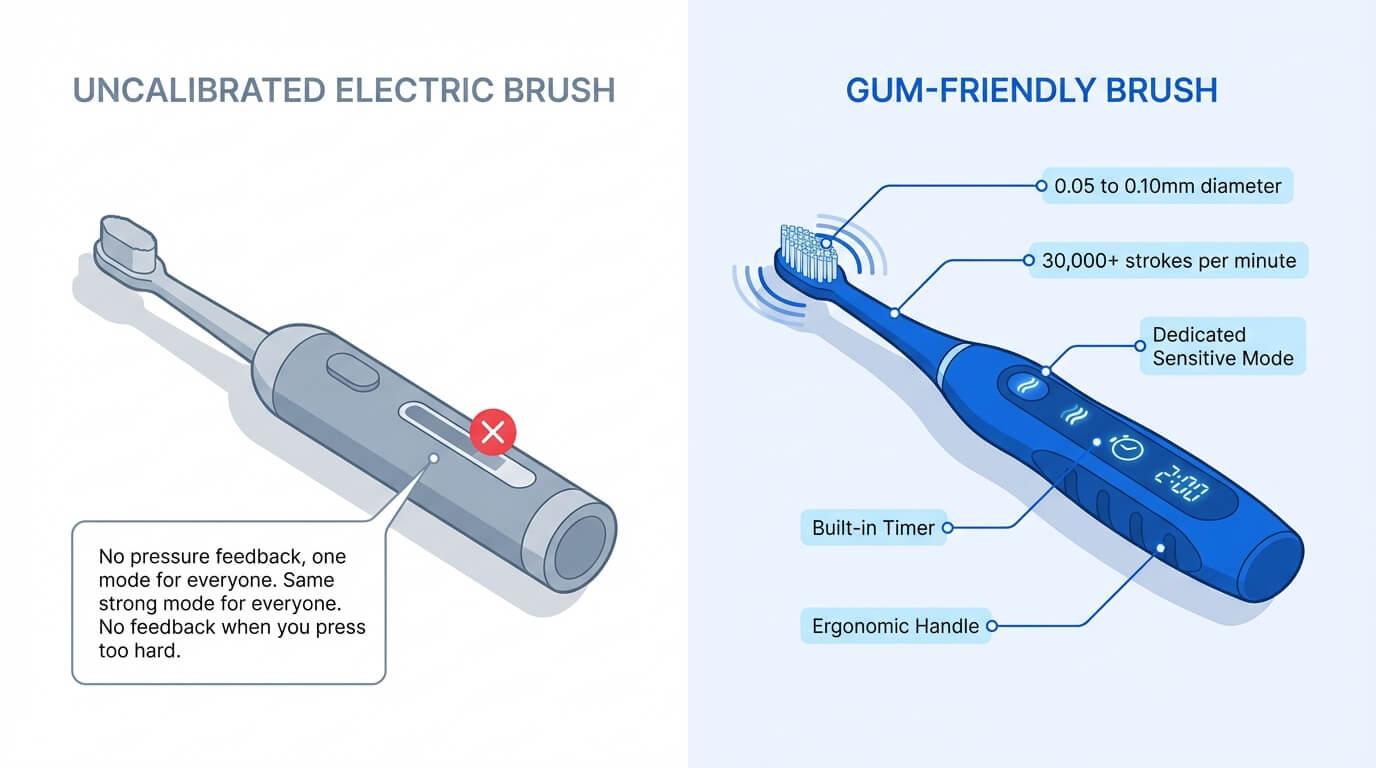
Many people follow all the standard advice: brush gently, use a soft-bristle toothbrush, and still have sore gums because their toothbrush itself is too intense or not designed for sensitivity.
Here is the problem: most manual and electric toothbrushes have 1 default intensity. Without pressure sensors or a true Sensitive mode, even "careful" brushing can be too harsh. Stiff or medium bristles, combined with high vibration, cause daily microtrauma to gum tissue.
Changing the tool is often more realistic than endlessly trying to "just brush softer," especially when you are half-asleep or rushing in the morning. The brush should adapt to your gums, not the other way around.
What a Gum-Friendly Toothbrush Should Do Differently
Core design features to look for:
-
Super-soft, finely tapered bristles that flex along the gum line (0.05 to 0.10mm diameter)
-
High-frequency sonic vibrations (30,000+ strokes per minute) that remove plaque without requiring pressure
-
A dedicated Sensitive mode with reduced intensity for days when your gums need extra care
-
A built-in timer to prevent overbrushing the same sore area
-
An ergonomic handle that encourages a light grip instead of a tight scrub grip
These features work together as a system to prevent gum irritation rather than relying on another tip to remember. The SNOW LED Whitening Electric Toothbrush combines sonic vibration with an advanced brush head design to deliver a thorough clean, designed with sensitive gum tissue in mind. Users who switch to properly designed brushes often report their gums stop hurting within 1 to 2 weeks: less bleeding, less post-brush soreness.
Home Care: What You Can Do Right Now for Sensitive Gums

Small, consistent changes beat drastic overhauls. Here is what you can start today:
-
Switch to a soft or ultra-soft brush with a true Sensitive or low-intensity mode
-
Use gentle circular motions at the gum line rather than sawing or scrubbing
-
Floss with the proper C-shape technique or use soft interdental brushes
-
Avoid aggressive brushing. Let the bristles do the work, not the pressure.
Supportive steps that soothe irritated gums during flare-ups:
-
Saltwater rinse: Mix 1/2 teaspoon of salt into a cup of warm water, swish gently for 30 seconds, and repeat 2 to 3 times daily. Salt water is a gentle, widely used home remedy that can temporarily soothe gum discomfort during flare-ups.
-
Antiseptic mouthwash: Choose alcohol-free versions that will not sting or dry out gum tissue. Alcohol-based rinses can irritate already sensitive gums.
-
Hydration: Drink more plain water throughout the day to support saliva production, which helps keep bacteria in your mouth under control.
-
Diet: Limit acidic foods and avoid constant sipping on sweetened drinks. A healthy diet rich in vitamin C supports your overall oral care routine.
Home remedies should show improvement within days to a couple of weeks. If they do not, treat them as a bridge to professional care, not a replacement for it.
When to See a Dentist About Sensitive Gums
See a dental professional if your gum sensitivity is:
-
Getting worse over time despite home care changes
-
Lasting more than 1 to 2 weeks despite proper brushing and flossing
-
Accompanied by warning signs: swelling, pus, loose teeth, fever, or signs of infection or gum disease
What a dentist might do:
-
Exams and X-rays to check bone levels and rule out more serious conditions
-
Professional cleaning or deep cleaning (scaling and root planing) to remove hardened plaque below the gum line
-
Review of your medical history, medications, and home routine to identify underlying contributors
-
Targeted treatments like antiseptic rinses, over-the-counter medications, or referral to a periodontist
Early intervention can often reverse gingivitis completely and prevent bone loss, making future gum sensitivity far less likely. Getting help early is a smart, proactive step. It is not a sign that you have failed at home care.
Final Words
Sensitive gums are common and, in most cases, very fixable. The causes, whether a harsh toothbrush, poor flossing technique, hormonal changes, or a systemic factor like diabetes or stress, are all identifiable. Most are reversible when you catch them early and use the right tools. What your gums are telling you is not that something is permanently wrong. It is that your current routine needs a small but meaningful adjustment.
SNOW is designed for exactly this. Explore the full collection built to support gum health and a more comfortable oral care routine.
Frequently Asked Questions About Gum Sensitivity
Have more questions? Here is what people ask us most about sensitive and sore gums.
Why are my gums so sensitive even though I brush gently?
Gums can still be sensitive despite gentle brushing if the toothbrush itself lacks a dedicated Sensitive mode or has bristles that are too stiff. Even careful brushing with an uncalibrated brush can cause micro-trauma to gum tissue with every use, leading to soreness and bleeding gums. Switching to a brush designed for sensitive gums often makes an immediate difference.
Can hormonal changes cause gum sensitivity?
Yes, hormonal fluctuations during puberty, menstruation, pregnancy, and menopause increase blood flow to the gums and amplify their reaction to plaque and bacteria, making them more tender and prone to sensitivity. Hormonal changes do not cause gum disease on their own, but they significantly lower the threshold at which your gums experience irritation.
How can I tell if my gum sensitivity is due to gingivitis or something more serious?
Gingivitis causes reversible redness, swelling, and bleeding of the gums, but no bone loss. If you notice persistent swelling, pus, loose teeth, or severe pain that does not improve, it may indicate periodontitis or another serious condition requiring prompt dental care. When in doubt, see a dental professional.
What role does my oral care routine play in gum sensitivity?
Your daily routine plays a central role in gum sensitivity. Aggressive brushing, improper flossing techniques, and using a toothbrush with stiff bristles or no pressure control are among the most common causes of gum irritation. Switching to a soft-bristle brush with a Sensitive mode and using gentle flossing methods can lead to noticeable improvement within days to 2 weeks.
When should I see a dentist about my sensitive gums?
See a dentist if gum sensitivity persists for more than 1 to 2 weeks despite proper home care, or if you experience swelling, pus, loose teeth, or fever. These signs may indicate infection or early-stage gum disease, which needs professional evaluation and treatment before it progresses.
Are there lifestyle factors that worsen gum sensitivity?
Yes. Uncontrolled diabetes, smoking, chronic stress, vitamin deficiencies (especially vitamin C and vitamin D), and consuming acidic or sugary foods can all increase inflammation and bacteria in your mouth, worsening gum sensitivity. Addressing these factors alongside good oral hygiene makes a meaningful difference in overall gum health.


