Why are your teeth sensitive? In most cases, it happens because thinned enamel or receding gums expose the softer dentin layer underneath, allowing hot, cold, and sweet stimuli to reach the nerve.
A 2024 multi-center European study confirmed that erosive tooth wear and gum recession are the two primary risk indicators for dentin hypersensitivity, and over 50% of adults experience it.
The sharp zing from iced coffee or cold air is one of the most common signs. At SNOW, we understand how quickly that pain disrupts simple moments.
Below, we break down the five root causes that all trace back to enamel loss, walk through a research-backed treatment hierarchy from desensitizing toothpastes to laser combination therapy, and explain how to keep whitening without triggering sensitivity.
If you’re looking for how to stop sensitive teeth pain immediately, the focus should be on protecting tooth enamel and calming the nerves. Below, we’ll walk you through what’s causing it and how to soothe sensitive teeth for lasting relief.
Key Takeaways
-
Tooth sensitivity primarily results from enamel erosion and gum recession, which expose the softer dentin layer, which contains nerve-connected tubules that trigger pain from hot, cold, sweet, or acidic stimuli.
-
Multiple causes, such as acidic foods, aggressive brushing, teeth grinding, and whitening products, converge on enamel wear, making enamel remineralization the essential focus for lasting relief.
-
Treatments combining desensitizing toothpastes (potassium nitrate, arginine, nano-hydroxyapatite), professional fluoride varnishes, and dental bonding offer effective ways to minimize sensitivity by rebuilding or protecting enamel.
-
Early dental evaluation is crucial for persistent or sudden sensitivity to rule out cavities, cracks, or gum disease and to implement personalized care that addresses the underlying cause rather than just masking symptoms.
What is tooth sensitivity, exactly?
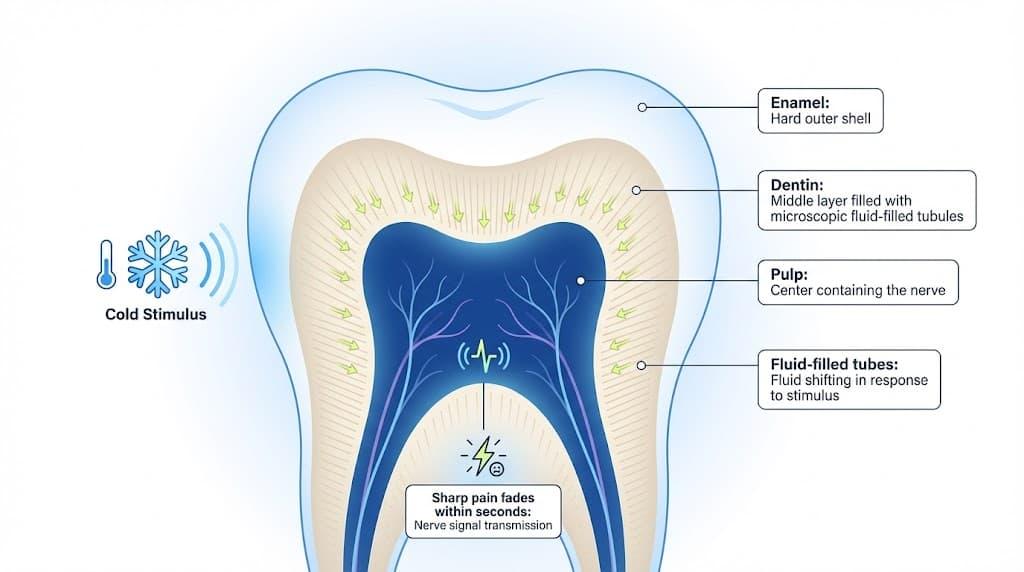
Tooth sensitivity, clinically called dentin hypersensitivity, is a brief, sharp pain that lasts only seconds and stops as soon as the hot, cold, or sweet stimulus is removed.
It is not a toothache.
A toothache lingers, throbs, and often signals decay or infection requiring restorative treatment. Sensitivity comes on fast and goes off fast, and that distinction matters because the treatment path is completely different: sensitivity responds to surface-level protection and desensitization, while a toothache typically requires a filling, crown, or root canal.
Your tooth has three layers: the outer shell of enamel (the hardest material in the body), a softer middle layer called dentin that is full of microscopic tubes leading to the nerves, and the pulp at the center where the nerve itself lives. When the outer layer thins, the middle layer does the talking.
A 2013 peer-reviewed study confirmed the hydrodynamic theory as the primary explanation for why exposed dentin hurts.
The mechanism works like this: dentin contains microscopic fluid-filled tubes, and when something hot, cold, or acidic reaches them, the fluid inside shifts. That movement triggers the nerve, and you feel it as a sharp pain that fades within seconds.
How Common Is Tooth Sensitivity? (And Should You Worry?)
More than half of adults experience dentin hypersensitivity, according to a 2023 seven-country European study of over 3,500 adults.
Prevalence estimates in systematic reviews have historically ranged from 10% to 57%, depending on the population studied and diagnostic criteria used. The 2023 Haleon study across seven European countries found that more than 50% of the 3,500+ adults surveyed had dentin hypersensitivity, making it one of the most common dental complaints.
You should not panic, but you also should not accept it as normal and move on.
A 2023 seven-country European study of over 3,500 adults found that more than 50% had dentin hypersensitivity, and 98% showed signs of enamel erosion.
Historical clinical data puts the figure around 57%. The most telling finding: people had been living with symptoms for over two years before seeking care. They normalized the pain when they should not have.
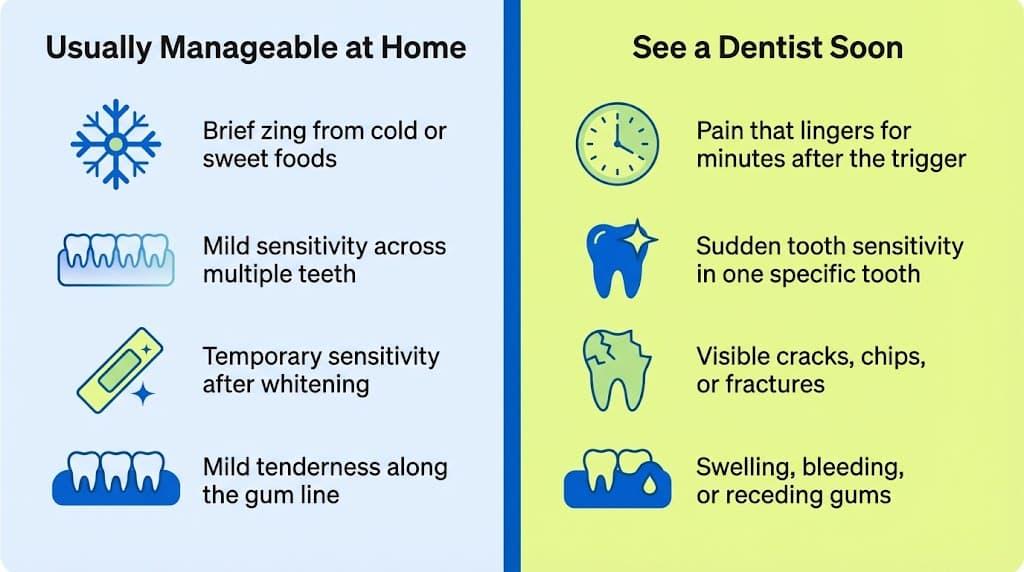
Here is a quick way to figure out which camp you are in:
Why Are My Teeth Sensitive? Main Causes That All Connect to Enamel Erosion
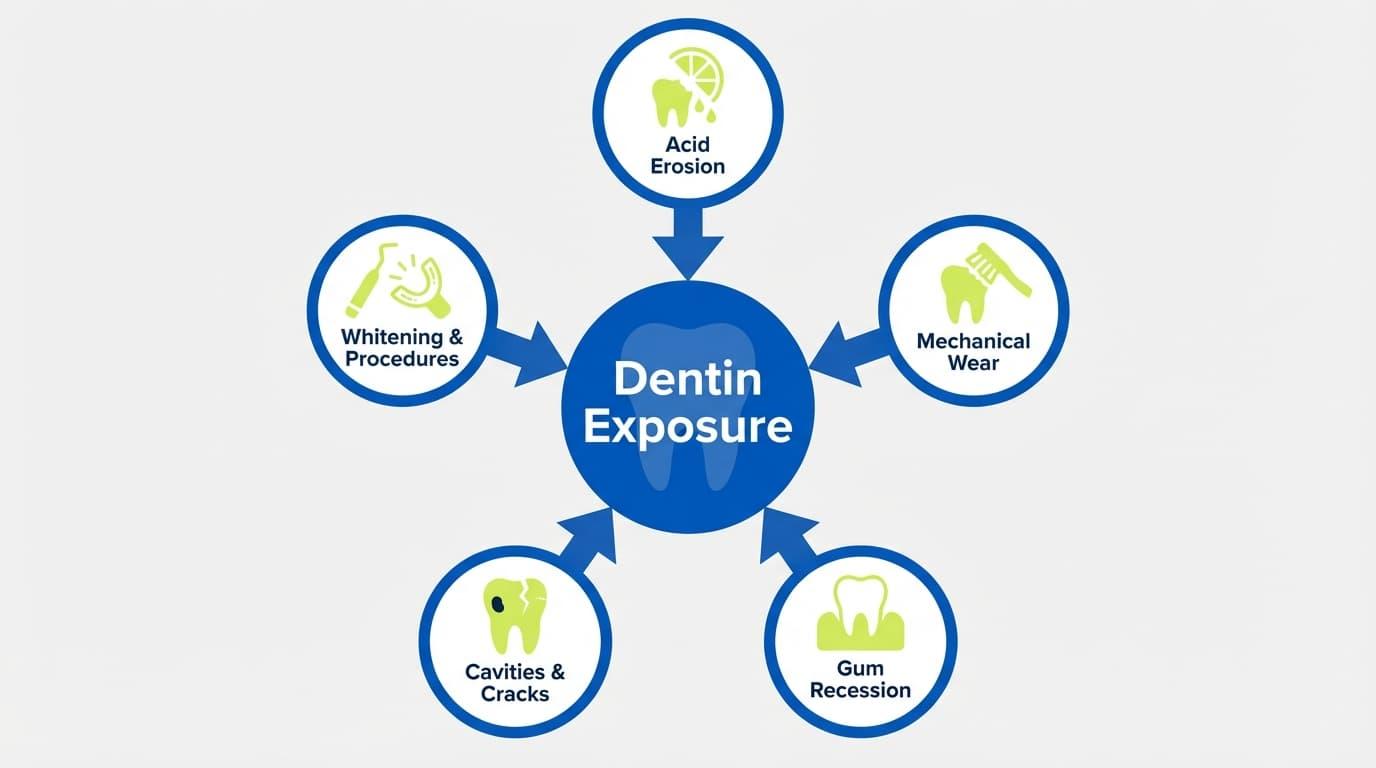
Most articles list causes like a grocery list. However, a 2024 multi-center EU study found that erosive tooth wear and gum recession are the two main risk indicators for dentin hypersensitivity. Ultimately, each of the causes below leads to enamel wear and dentin exposure.
Enamel Erosion from Acids
Acid erosion is one of the two primary drivers of sensitive teeth identified by a 2024 multi-center European study, and acids come from more sources than most people expect.
-
External acids: Citrus fruits, sodas, energy drinks, wine, and vinegar-based dressings gradually dissolve enamel minerals with repeated exposure.
-
Internal acids: Acid reflux and GERD repeatedly bring stomach acid up, eroding the inner tooth surfaces in patterns distinct from dietary erosion.
-
Acidic mouthwashes: Some have a low pH that can contribute to enamel erosion, especially when used daily.
Where enamel erosion appears often points to its cause. Dietary acids from citrus, soda, and energy drinks typically affect the upper front teeth and biting edges. Acid reflux creates a different pattern: erosion concentrated on the inner surfaces of the back teeth. If your sensitive areas match either pattern, acid exposure is the likely driver.
Mechanical Wear: Brushing Hard, Abrasive Products, and Teeth Grinding
Physical force removes tooth enamel just as effectively as acid does. Here is how each one works:
-
Aggressive brushing: A hard-bristled brush or abrasive toothpaste physically scrapes enamel away at the gum line. Use a soft-bristle toothbrush instead, and let the bristles do the work rather than applying pressure.
-
Teeth grinding (bruxism): Creates constant pressure on enamel, which thins it over time and produces microcracks. Watch for flat chewing edges, jaw soreness in the morning, or reports from a partner about grinding sounds during sleep.
There is a compounding effect worth understanding: research on erosive-abrasive tooth wear shows that acid-softened enamel wears away at a measurably faster rate under mechanical force than healthy enamel does.
If you grind regularly and consume acidic foods and drinks throughout the day, the combined damage accelerates far beyond what either factor alone would produce.
Gum Recession and Exposed Roots
Tooth roots are not covered by thick enamel. They are protected by gum tissue. When gums pull back due to periodontal disease, overbrushing, or bite issues, those exposed tooth roots suddenly face everything: cold air, acidic foods, and physical contact.
Gum recession explains why tooth sensitivity often concentrates at the gum line on lower front teeth and canines. Mild recession responds well to desensitizing toothpaste. Severe receding gums may require gum grafts rather than a change in toothpaste.
Cavities, Cracked Teeth, and Leaking Fillings
Generalized sensitivity often signals enamel erosion, while sudden sensitivity in one tooth, especially sharp pain when biting, may suggest decay, a crack, or a failing filling.
These conditions create a direct pathway to the tooth's sensitive inner parts and require prompt evaluation. Home treatment will not resolve a cracked tooth or an active cavity. If sensitivity is localized and sudden, get it checked.
Whitening Products and Recent Dental Procedures
High-peroxide whitening systems can temporarily worsen tooth sensitivity by dehydrating enamel and leaving dentin tubules more reactive. Not all teeth whitening works the same way, though. Some systems strip enamel without any surface support; others include ingredients that fill surface gaps and protect the tooth during the whitening process.
Recent dental procedures, such as cleanings, fillings, and extractions, can also cause temporary sensitivity that lasts a few days to two weeks. If pain gets worse rather than better after a procedure, call your dentist.
Is Sensitive Enamel permanent, Or Can It Get Better?

Dentist-guided treatments produced measurable improvement in about 60% of patients, according to a 2017 National Dental Practice-Based Research Network study. Consistent at-home care with desensitizing toothpastes pushes that number even higher.
The solution is targeting the root cause, not just masking symptoms. Potassium nitrate works by blocking nerve signals so pain impulses never fire.
Arginine and nano-hydroxyapatite take the opposite approach, physically rebuilding the tooth surface by sealing exposed tubules or filling micro-defects in enamel. Restoring the protective layer interrupts the pain at its source rather than numbing it.
Sensitive teeth do not always indicate a cavity. Most cases are caused by general enamel wear or gum recession across multiple teeth, not localized decay.
The diagnostic clue: sensitivity spread across several teeth that responds to temperature typically points to enamel loss, while sharp pain in a single tooth, especially when biting down, is more likely a cavity or crack that needs professional evaluation.
Everyday Habits That Quietly Make Your Teeth More Sensitive
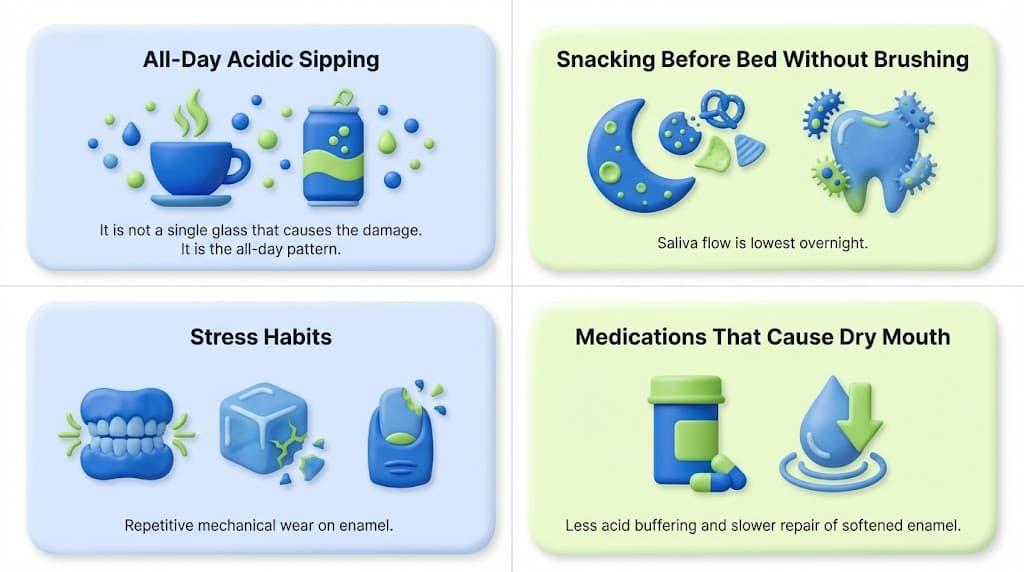
A cracked tooth gets noticed immediately. But the daily habits that thin your enamel grain by grain over months — the all-morning coffee sipping, the stress clenching, the bedtime snack without brushing — those go unnoticed until the sensitivity arrives.
These are the patterns worth watching:
-
Frequent sipping of acidic drinks: Nursing coffee, sparkling water with citrus, or energy drinks all morning keeps tooth enamel in a near-constant softened state. It is not a single glass that causes the damage. It is the all-day pattern.
-
Snacking before bed without brushing: Food debris from sugary and starchy foods feeds acid-producing bacteria overnight, right when saliva flow is lowest, and the mouth's natural buffering capacity is weakest.
-
Stress habits: Clenching the jaw during the day, chewing ice, biting fingernails, or using teeth to open packages create repetitive mechanical wear on enamel.
-
Certain medications: Antihistamines, antidepressants, and blood pressure medications can cause dry mouth by reducing saliva. Less saliva means less acid buffering and slower repair of softened enamel.
If whitening is part of your routine but sensitivity keeps following you, SNOW Overnight Sensitive Teeth Whitening Pen is built for that problem. It applies a hydroxyapatite formula before bed and works overnight, gradually whitening while remaining gentle on the tooth surface. No trays, no strips, and no rinsing needed. It is designed specifically for people who want to keep whitening without the discomfort that typically follows high-peroxide systems.
Get the SNOW Overnight Sensitive Pen
How to Calm Sensitive Teeth: Proven Treatment Options
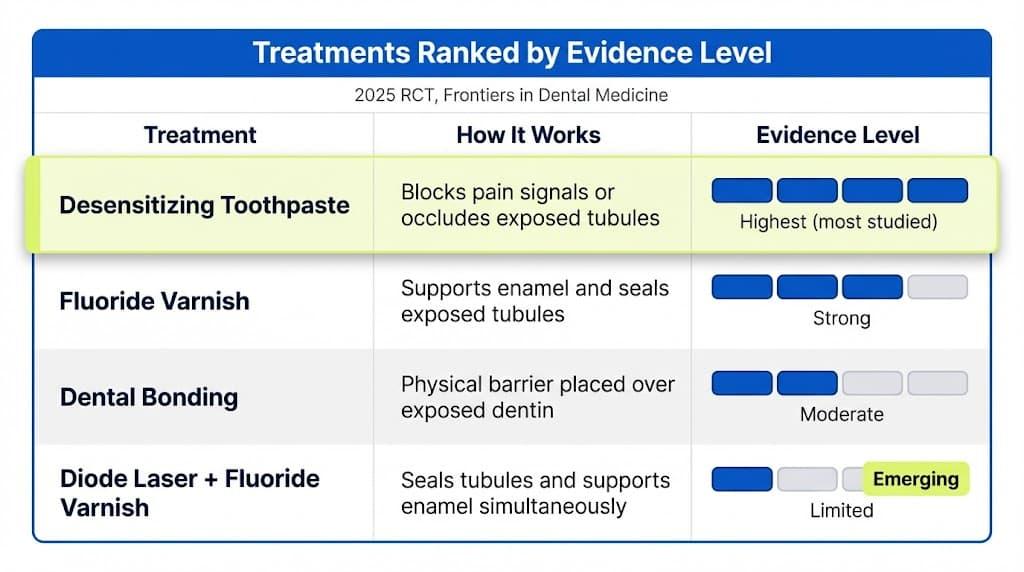
Treatments range from straightforward at-home care to in-office procedures. A 2025 randomized controlled trial published in Frontiers found that combining a diode laser with fluoride varnish produced the greatest reduction in sensitivity among the options tested, reinforcing that combination approaches tend to outperform any single treatment.
Here is what the evidence actually says, ranked by how well it is studied:

Desensitizing and Protective Toothpastes
Not all desensitizing toothpastes work the same way. The active ingredient determines the mechanism.
Potassium nitrate blocks pain signals by raising potassium ion levels around nerve endings, reducing the likelihood that they will fire. It takes 2 to 4 weeks of consistent use to reach full effect.
Arginine-based formulas physically occlude dentinal tubules with a calcium-containing plug. According to a 2022 arginine toothpaste study, these formulas produced 72-84% immediate pain reduction, making them among the fastest-acting options available.
Nano-hydroxyapatite is a bio-identical mineral that integrates into micro-defects on the tooth surface, filling surface gaps in the protective layer rather than just blocking nerve signals.
A 2019 systematic review in the Journal of Dentistry found that hydroxyapatite toothpastes were comparable to fluoride in remineralizing early enamel lesions, supporting their use as both a sensitivity treatment and an enamel repair agent.
Brush gently twice daily, avoid rinsing aggressively right after brushing, and give any desensitizing toothpaste at least two to four weeks before judging whether it is working. Good oral hygiene paired with the right toothpaste is more effective than switching products every few days.
Professional Fluoride Treatments, Varnishes, and Dental Bonding
When at-home products are not enough, in-office options step in. Professional fluoride varnish delivers a concentrated application directly to sensitive areas and occludes tubules at a level that over-the-counter products cannot match.
Dental bonding places a resin barrier directly over exposed roots or worn enamel areas, providing fast, lasting relief.
For severe gum recession with exposed tooth roots, gum grafts address the structural cause of sensitivity rather than just the symptom.
Emerging Options: Lasers and Combination Therapies
A 2025 randomized controlled trial published in Frontiers in Dental Medicine found that a diode laser combined with fluoride varnish produced the greatest reduction in sensitivity among all treatment options tested. The laser seals tubules at a microscopic level while the varnish supports the enamel surface.
The laser seals tubules at a microscopic level while the varnish supports the enamel surface.
Long-term data beyond 12 months remain limited, but this combination is now available for patients who have not responded to other treatments.
When Surgery Is the Right Answer
Two situations call for surgical intervention.
First, a severe gum recession that has exposed significant root surface may require gum grafts to restore tissue and cover the roots.
Second, when persistent sensitivity points to damaged nerve tissue or deep decay, root canal therapy removes the affected nerve and permanently ends that source of pain.
Root canal treatment is a last resort, not a first step.
It comes with three professional-grade serums and an LED accelerator light, and has earned over 5,000 verified five-star reviews from customers who use it at home.
It comes with three professional-grade serums and an LED accelerator light, and has earned over 5,600 verified five-star reviews. The formulas are designed to be gentler on the tooth surface than standard high-peroxide strips, making this a practical choice for anyone who has experienced whitening-triggered discomfort and wants real results without repeating that cycle.
Get the SNOW Diamond Series Kit
Can Whitening and Sensitive Teeth Ever Coexist?
Yes. But it depends entirely on the teeth whitening system you use.
High-peroxide systems that dehydrate enamel have made whitening synonymous with pain for many people. That is a formula problem, not a teeth problem. The question to ask about any whitening product is: Does it just bleach, or does it also support the tooth surface during the process?
Whitening systems that include nano-hydroxyapatite and potassium nitrate in the serum address both sides. The whitening agent lifts stains, while the protective ingredients fill surface gaps and help minimize sensitivity. Spacing sessions every other day rather than daily also significantly reduces cumulative irritation.
SNOW Dissolving Teeth Whitening Strips solve a problem that standard strips create. Unlike traditional strips that peel off and sometimes pull at sensitive areas along the gum line, SNOW's Dissolving Strips adhere, whiten, and dissolve completely on their own.
The formula includes hydroxyapatite to support the tooth surface during whitening, and its dissolving format helps reduce irritation that strip removal can cause.
Consistently rated 5 stars by verified buyers, they are a gentler format for anyone who has had bad experiences with conventional whitening strips.
Get SNOW Dissolving Whitening Strips
When to See a Dentist About Sensitive Teeth

Most sensitive teeth cases are manageable at home. Some of them are not. Here is when to stop self-treating and call a dentist:
-
Sudden sensitivity in one specific tooth that was not sensitive before
-
Pain that lingers for more than a few seconds after the trigger is removed
-
Persistent sensitivity that does not improve after two weeks of consistent at-home treatment
-
Visible cracks, chips, or fractures on any tooth
-
Swelling, bleeding, or receding gums around one or more teeth
-
Sharp pain, specifically when biting down on food, signals a possible cracked tooth or cavity
Early action means simpler, less invasive treatments. At a sensitivity-focused dental visit, expect a full history, a targeted exam, cold and air stimulus testing, and possibly X-rays. From there, your dentist can put together a personalized plan that addresses the underlying cause rather than just managing the symptom.
If you want to add surface support to your daily routine without changing everything, SNOW Magic Teeth Whitening Powder makes it simple. Mix a small amount with your regular toothpaste and brush as normal. The formula uses color-correcting technology to tone down yellow stains on contact, while nano-hydroxyapatite gradually fills microscopic surface gaps. No new tools, no extra steps. Rated 4.8 stars across 160 verified reviews.
Get the SNOW Magic Whitening Powder
Final Thoughts
Tooth sensitivity affects more than half of adults, but the research is clear: it responds to treatment. Every cause covered in this article — acid erosion, mechanical wear, gum recession, cavities, and whitening irritation — traces back to exposed dentin.
The treatment hierarchy follows the same logic: start with desensitizing toothpastes that block nerve signals or seal tubules, step up to professional fluoride varnishes or bonding if needed, and reserve surgical options for structural damage. Matching the treatment to the specific cause is what produces lasting results.
If you need to know how to stop sensitive teeth pain immediately, start simple. Use a sensitive toothpaste, avoid very hot or cold foods, and pause whitening briefly to soothe sensitive teeth. From there, focus on long-term care, such as gentle brushing, limiting acidic foods, and choosing products made for sensitive teeth.
At SNOW, we take a sensitivity-first approach by pairing whitening with ingredients that help support tooth enamel. Most people see improvement within a few weeks. If tooth pain continues or feels severe, it’s time to see a dentist.
Frequently Asked Questions
Got questions about sensitive teeth and tooth pain? Here are quick, clear answers to help you find relief fast.
Why do my teeth feel sensitive to hot, cold, or sweet foods?
Teeth feel sensitive to hot, cold, or sweet foods when tooth enamel wears down or gums recede. This exposes the inner layer of the tooth, leading to tooth sensitivity and sharp pain when triggered. Sensitive teeth react more easily to temperature and sugar.
Can tooth sensitivity be reversed or treated?
Yes. About 60% of patients in a National Dental Practice-Based Research Network study improved with dentist-guided treatments, and many more see results with consistent at-home care. Desensitizing toothpastes containing potassium nitrate block pain signals over two to four weeks, while arginine-based formulas physically seal exposed tubules for faster relief. The key is matching the treatment to the cause rather than masking symptoms.
What causes tooth enamel to erode and lead to sensitivity?
Tooth enamel can erode due to acidic foods and drinks, brushing too hard, teeth grinding, and some whitening products. This erosion leads to tooth sensitivity and increases the risk of tooth pain. Protecting enamel helps prevent sensitive teeth.
Are whitening products safe if I have sensitive teeth?
Whitening products can be safe for sensitive teeth when they are designed to support tooth enamel. Some formulas can increase tooth sensitivity, but better options are made to soothe sensitive teeth during use. Choosing the right system makes a big difference.
When should I see a dentist about my tooth sensitivity?
You should see a dentist about tooth sensitivity if the pain lasts more than 2 weeks, is severe, or affects a specific tooth. Signs like swelling or gum disease also need attention. Persistent sensitive teeth may require professional care.
How can I prevent my teeth from becoming more sensitive?
You can prevent sensitive teeth by brushing gently with a soft toothbrush, limiting acidic foods, and protecting tooth enamel daily. Using products made to soothe sensitive teeth can also reduce tooth sensitivity over time. Consistent habits help prevent tooth pain.
