Sensitive teeth pain stops fastest with desensitizing toothpaste applied directly to the affected tooth, a warm salt water rinse, and avoiding hot, cold, and acidic foods for 24 to 48 hours. These three steps calm nerve activity within minutes to hours.
At SNOW — where our sensitivity-safe whitening formulas have completed over 100 million treatments across 2.4 million customers — we see this flare-up pattern constantly, and these steps work.
This article covers nine immediate at-home remedies with application instructions, what distinguishes whitening-triggered sensitivity from everyday sensitivity, the underlying causes driving persistent pain (enamel erosion, gum recession, bruxism, cracked teeth), a clear decision framework for when to see a dentist versus managing at home, and the long-term treatments clinically shown to reduce dentin hypersensitivity over two to four weeks. If your sensitivity followed a whitening session, there is a specific 72-hour protocol covered in detail below.
Key Takeaways:
-
Use desensitizing toothpaste with potassium nitrate or stannous fluoride as a fast-acting spot treatment to block pain signals from exposed dentin.
-
Warm salt water rinses and cold compresses reduce gum inflammation and nerve irritation, providing quick relief within minutes to hours.
-
Avoid extreme temperatures, acidic foods, and sweets for 24–48 hours to prevent aggravating sensitive teeth while they heal.
-
If sensitivity is triggered by whitening products, switch to formulas that include enamel-strengthening ingredients such as potassium nitrate and nano-hydroxyapatite to prevent recurring pain cycles.
-
Consult a dentist promptly if the pain is severe, persists beyond 2 weeks, or is accompanied by signs of infection or structural damage.
Why Your Teeth Are Sensitive: What Is Actually Happening
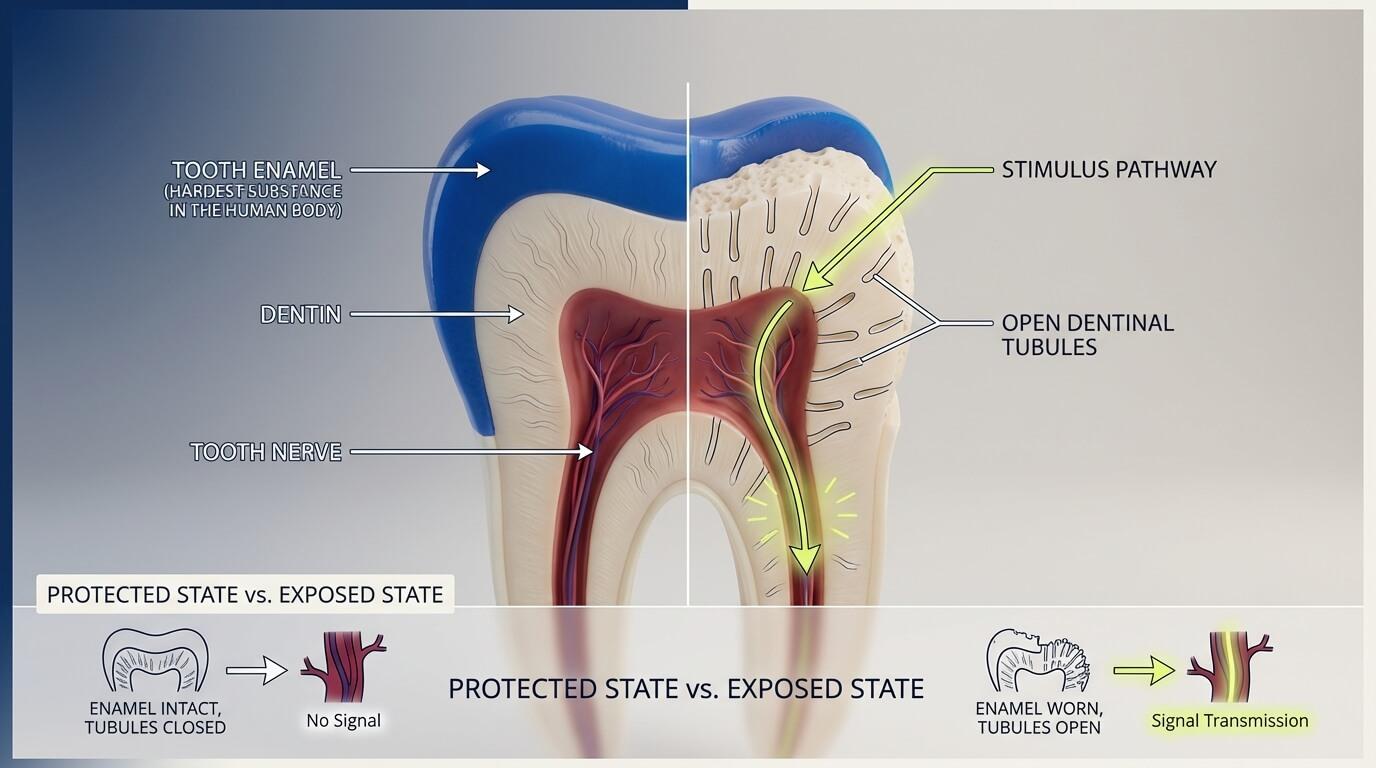
If you want to stop sensitive teeth pain for good, it helps to understand the basics of what is going wrong inside the tooth. It is simpler than it sounds.
Teeth have two structural layers: the outer shell of tooth enamel (the hardest substance in the human body) and an inner layer of dentin, packed with microscopic tubes called dentinal tubules that connect directly to the tooth nerve.
This architecture matters because once enamel wears down or gums recede, those tubules are exposed — and every cold drink, hot coffee, or sweet food sends a signal straight to the nerve.
Tooth sensitivity occurs when enamel wears down or the gums recede, exposing the dentin underneath. Once those tubules are open, cold temperatures, hot drinks, sweet or acidic foods, and even cold air go straight to the nerve. That sharp, electric zap you feel? That is your nerve reacting to a stimulus it was never supposed to reach.
Why Whitening-Triggered Tooth Pain Feels Sharper
Most sensitivity builds slowly over months. Whitening-triggered tooth sensitivity is different. High-concentration peroxide penetrates enamel to lift stains but also temporarily increases tooth permeability (2018, Journal of Evidence-Based Dental Practice), leaving dentin tubules wide open and reactive to everything. The result is a sudden, intense flare that catches most people off guard.
The root problem is not whitening itself. It is using a whitening formula with no built-in protection. When you keep whitening with an unprotected product, you keep reopening the same pathways, and the tooth pain cycle repeats every time.
How to Stop Sensitive Teeth Pain Immediately at Home
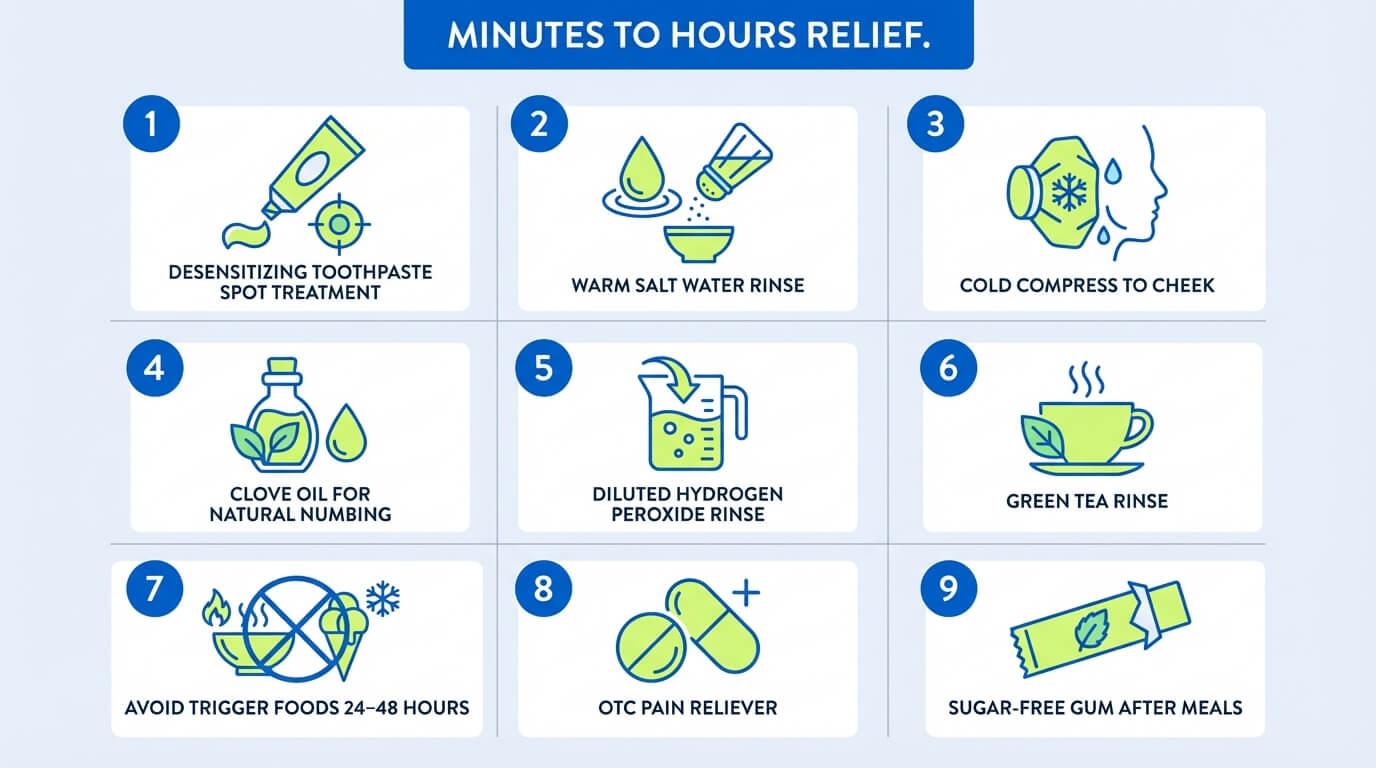
These nine at-home steps reduce sensitive teeth pain within minutes to hours without a dentist visit. They work by calming nerve activity, reducing gum inflammation, and blocking pain signals at the dentin tubule level — buying real relief while longer-term treatments build up over 2 to 4 weeks.
1. Use Desensitizing Toothpaste as a Spot Treatment
Desensitizing toothpaste contains ingredients like potassium nitrate or stannous fluoride that block pain signals from reaching the tooth nerve.
Most people brush with desensitizing toothpaste and move on — that reduces sensitivity over time. But for immediate relief, there is a faster method: apply a pea-sized amount to a clean finger or cotton ball, press it directly onto the affected tooth, and let it sit for 2 to 5 minutes without rinsing. Repeat up to 3 times daily during a flare-up.
But for immediate relief, there is a faster method:
-
Squeeze a pea-sized amount onto a clean finger or cotton ball
-
Press it directly onto the affected tooth
-
Let it sit for 2 to 5 minutes without rinsing
-
Rinse gently after. Repeat up to 3 times a day during a flare-up
A 2023 randomized clinical trial published in Scientific Reports found that consistent use of desensitizing toothpaste significantly reduced dentin hypersensitivity scores within 2 to 4 weeks.
Using it as a spot treatment means you get some of that blocking action right at the source, right away.
For whitening-triggered sensitivity, formulas that combine hydroxyapatite with potassium nitrate address both problems simultaneously — the hydroxyapatite fills exposed dentinal tubules while the whitening agent lifts stains.
The SNOW Overnight Sensitive Whitening Pen uses this dual-action approach: apply before bed, no rinsing required, and let the hydroxyapatite-based formula support enamel remineralization while you sleep.
Get the SNOW Overnight Sensitive Whitening Pen
2. Rinse with Warm Salt Water
Salt water is one of the oldest oral remedies, and it holds up. Here is the how and why:
-
A 2021 study in the Journal of Indian Society of Periodontology found that salt water rinse showed anti-inflammatory effects comparable to chlorhexidine mouthwash after periodontal procedures
-
Salt draws fluid out of inflamed gum tissue, reducing swelling and calming gum irritation around sensitive teeth
-
Mix 1 teaspoon of table salt into 8 oz of warm water. Swish gently for 30 seconds. Spit and repeat up to 3 times daily
-
Use warm water, not hot. Hot water triggers pain in teeth sensitive to temperature
3. Apply a Cold Compress to Your Cheek
A cold compress slows nerve conduction and reduces inflammation. The keyword is outside. Here is how to use it correctly:
-
Wrap a cold pack or a bag of frozen peas in a thin cloth
-
Hold it against your cheek directly over the painful area for 10 to 15 minutes
-
Wait at least 10 minutes between uses
-
Never put ice on the affected tooth or in your mouth. Cold contact on teeth sensitive to cold temperatures makes it significantly worse
4. Try Clove Oil for Natural Numbing
Clove oil has been used in clinical dentistry for over a century, and its active compound, eugenol, is the reason. According to the NCBI LiverTox database, eugenol has local anesthetic and antiseptic properties that block nerve signals and reduce inflammation in dental tissue. Here is how to use it safely:
-
Dilute 1 drop of clove oil in 4 to 5 drops of olive or coconut oil
-
Apply to a clean cotton ball and hold it on the sore tooth or along the gum line for 5 to 10 minutes
-
Remove and rinse. Never swallow
-
Never apply undiluted clove oil. It will cause further irritation or burns to soft tissue
-
Use this as an emergency tool for sudden flare-ups, not as a daily mouth rinse
5. Try a Diluted Hydrogen Peroxide Rinse
A diluted hydrogen peroxide rinse reduces the oral bacteria and gum inflammation that directly intensify nerve sensitivity in exposed dentin.
Mix equal parts 3% hydrogen peroxide and water, swish for 30 seconds, and spit — never swallow. Limit use to 2–3 times per week during active flare-ups only; daily application irritates oral mucosa and disrupts the microbiome balance that supports gum health. Pair it with desensitizing toothpaste for a combined antibacterial and nerve-blocking effect.
6. Add a Green Tea Rinse to Your Routine
Green tea polyphenols deliver documented anti-inflammatory and antimicrobial action (Narotzki et al., 2012) that reduces gum inflammation contributing to tooth sensitivity.
Brew unsweetened green tea, cool to room temperature, and swish for 30 seconds — this pairs with desensitizing toothpaste as a low-irritation complement during active flare-ups.
7. Avoid Trigger Foods and Drinks for 24 to 48 Hours
Exposed dentin overreacts to extremes. Give it a break. Here is what to skip and what to eat instead:
 Every time you test the sore tooth with cold or sweet stimuli, you reset the pain clock. A day or two of boring eating pays off.
Every time you test the sore tooth with cold or sweet stimuli, you reset the pain clock. A day or two of boring eating pays off.
8. Take an OTC Pain Reliever if Needed
Ibuprofen (an NSAID) reduces tooth pain by suppressing prostaglandins, the signaling molecules that amplify nerve sensitivity during inflammation — making it more effective than acetaminophen for inflammation-driven tooth sensitivity specifically.
Follow standard package dosing and never crush pills onto gums, as this burns soft tissue. If pain requires medication beyond 48 hours, home treatment is not sufficient: see a dentist to rule out a cracked tooth, infection, or pulp involvement.
9. Chew Sugar-Free Gum After Meals
Chewing sugar-free gum boosts saliva production, which neutralizes acids and reduces how often triggers cause discomfort after meals.
Saliva is your mouth's built-in acid buffer. More saliva means a less acidic environment around sensitive teeth, fewer trigger moments, and slower enamel wear over time.
This single post-meal habit reduces acid dwell time on enamel — one of the lowest-effort, highest-frequency protective actions available outside of brushing.
Why Whitening-Triggered Sensitive Teeth Pain Feels Different
Post-whitening tooth pain has a specific cause, and once you understand it, fixing it becomes much simpler.
Standard whitening products use peroxide to lift stains. As a side effect, peroxide temporarily increases enamel permeability, leaving dentin tubules wide open and reactive. Add in cold air, cold drinks, or anything acidic or sweet, and the nerve fires hard. That is why whitening-triggered tooth sensitivity often feels more intense and more sudden than regular sensitive tooth pain.
A 2021 clinical study published in BDJ Open found that whitening formulas combining nano-hydroxyapatite with potassium nitrate significantly reduced dentin hypersensitivity scores compared to placebo — supporting the case for protective-ingredient formulas over standard high-peroxide products.
When these ingredients are built into the whitening serum, enamel protection and whitening occur simultaneously rather than working against each other.
What to Do If Sensitivity Came from Last Night's Whitening Session
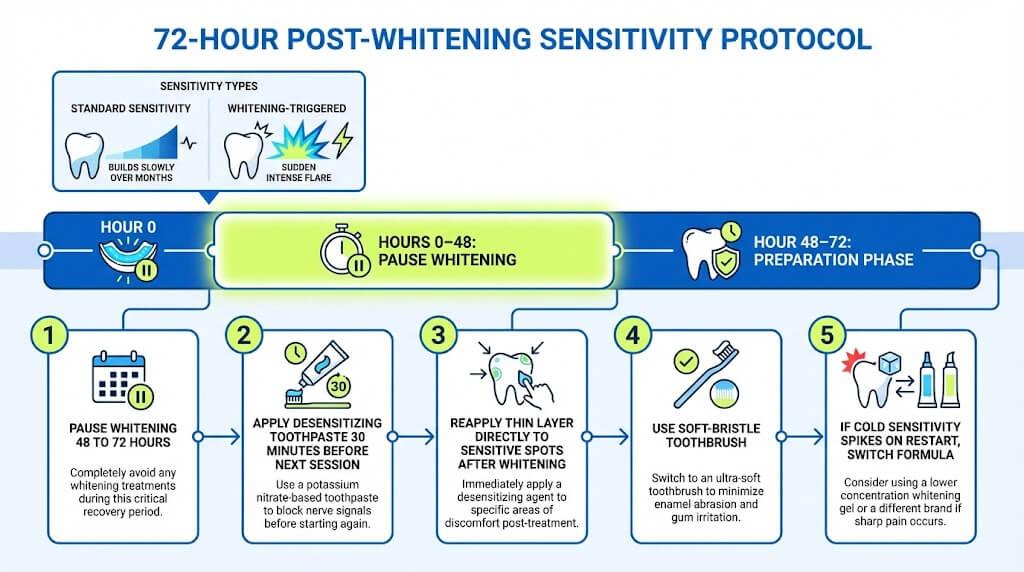
Here is exactly what to do in the next 72 hours:
-
Pause whitening for 48 to 72 hours. Skip at least 2 to 3 sessions. Continuing during active pain deepens the problem
-
Apply desensitizing toothpaste 30 minutes before your next session once you resume
-
Reapply a thin layer directly to sensitive spots right after whitening as a protective buffer
-
Use a soft-bristle toothbrush, not a medium or hard one, when applying toothpaste near sensitive areas
-
If cold sensitivity spikes again the moment you restart, that is your formula, not your teeth. Time to switch products
The SNOW Diamond Series is SNOW's flagship whitening system, with over 5,600 verified buyer reviews and a 4.9-star rating (as of 2025). It comes with three professional-grade serums and an LED accelerator light.
It comes with three professional-grade serums and an LED accelerator light. Unlike standard high-peroxide strips that leave teeth sensitive for days, this kit is built to whiten without triggering repeated sensitivity. The serum formulas are specifically developed for people who want real results without the tooth pain that follows.
Get the SNOW Diamond Series Whitening Kit
What Causes Sensitive Teeth: The Full Picture
Whitening is often the trigger, but it is rarely the only cause. Most people dealing with persistent tooth sensitivity have underlying issues that whitening simply amplifies.
Here is a breakdown of the main causes and what each one does:
Enamel Erosion
Tooth enamel is strong, but it is not indestructible. Acidic foods and drinks, such as soda, energy drinks, citrus fruits, and wine, gradually break it down. So does enamel wear from teeth grinding and aggressive brushing, as confirmed in multiple studies on enamel erosion patterns. Once enamel is gone, it does not grow back. That is why prevention is easier than repair.
Gum Recession and Receding Gums
When receding gums pull away from the tooth, they expose the root surface. Unlike the crown of the tooth, roots have no enamel. They are covered by cementum, a much softer material that provides almost no protection against temperature or pressure. Gum recession is a direct route to severe, hard-to-treat tooth sensitivity.
Teeth Grinding (Bruxism)
Teeth grinding puts extreme repetitive force on enamel, wearing it down significantly over time. Many people do not even know they grind until a dentist notices the damage. If grinding is a factor, a custom night guard is one of the most effective interventions you can get. Protect the enamel you have left.
Plaque Buildup and Gum Disease
Plaque buildup that is not removed consistently leads to gum inflammation and, eventually, gum disease. Both conditions cause gum tissue to break down and recede, exposing more tooth roots over time. This is why proper brushing and flossing are not just about clean teeth. They are about keeping gums healthy and in place.
Cracked Teeth and Recent Dental Procedures
Cracked teeth bypass enamel entirely, creating a direct path for stimuli to reach the nerve. Cracks can come from grinding, biting hard foods, or impact. Sharp, sudden, and localized sensitivity to one specific tooth often indicates a crack. Recent dental procedures, such as fillings and cleanings, can also cause temporary sensitivity for a few days while the tooth settles.
When to Handle It at Home vs. When to See a Dentist

Not all sensitive teeth pain is created equal. Some of it you can absolutely handle on your own.
Some of it needs professional dental care and a dentist's tools. Here is how to tell the difference:
 Clinical studies confirm that consistent use of a desensitizing toothpaste for 2 to 4 weeks produces meaningful sensitivity reduction in most people. Track your pain week by week. If it is improving, keep going. If it is getting worse, book an appointment. When in doubt, see a dentist.
Clinical studies confirm that consistent use of a desensitizing toothpaste for 2 to 4 weeks produces meaningful sensitivity reduction in most people. Track your pain week by week. If it is improving, keep going. If it is getting worse, book an appointment. When in doubt, see a dentist.
A dentist can provide professional fluoride treatments, dental bonding to cover exposed root surfaces, or assess whether tooth decay or a cracked tooth is driving the problem. Some situations are beyond the reach of any toothpaste.
Proven Treatments That Reduce Tooth Pain for the Long Term
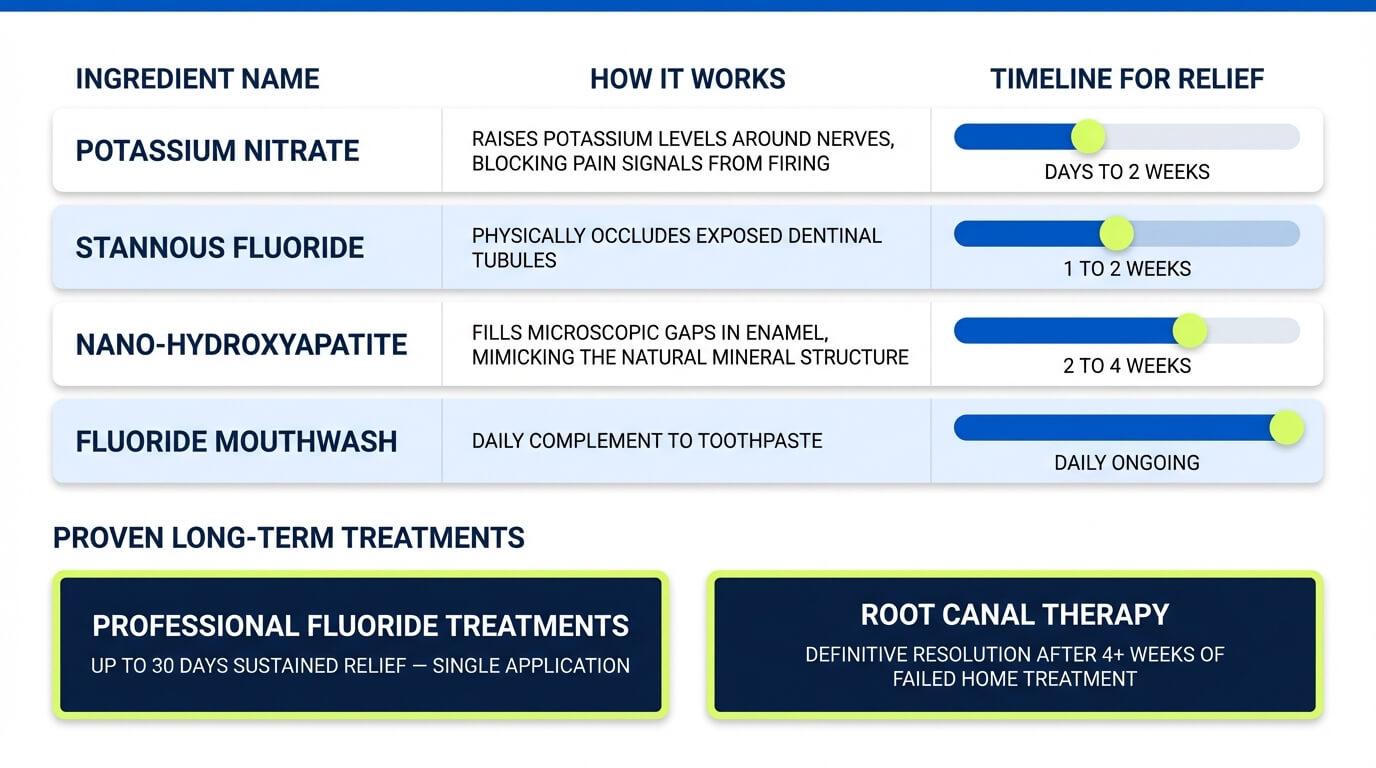
Immediate relief steps calm the storm. These evidence-backed options are what actually fortify your teeth over time.
Desensitizing Toothpaste and Fluoride Mouthwash
This is your most accessible and consistent long-term tool. Here is what the active ingredients actually do:

A 2024 randomized controlled trial published in Compendium of Continuing Education in Dentistry found significant reductions in dentin hypersensitivity from day 1 through day 7 with a stannous fluoride formula stabilized with nitrate and phosphates (SNAP), compared to a control.
Use desensitizing toothpaste consistently for 2 to 4 weeks before evaluating results. Pair desensitizing toothpaste with a fluoride mouthwash at night, when saliva flow is lowest, and fluoride dwells on enamel surfaces longest without dilution.
Use desensitizing toothpaste consistently for 2 to 4 weeks before judging results. Pair it with a fluoride rinse at night for the strongest combined effect.
Professional Fluoride Treatments and Dental Bonding
When desensitizing toothpaste is insufficient, a dentist can apply concentrated fluoride varnish directly to exposed dentin — a 2024 clinical study (PMC11196028) found that in-office fluoride agents and resin-based bonding materials each produced sustained sensitivity reduction for up to 30 days after a single application.
For exposed root surfaces that don't respond to remineralization, dental bonding physically seals the surface, blocking stimulus pathways without requiring ongoing maintenance. The key differentiator: fluoride works via remineralization; bonding works via mechanical occlusion.
Root Canal Therapy for Severe Cases
Root canal therapy is indicated when sensitivity is severe, localized to a single tooth, and diagnosed as irreversible pulpitis — meaning the nerve is inflamed beyond the point of self-repair.
The procedure removes the nerve entirely, permanently eliminating that pain source. It is not a first-line option, but it is the definitive resolution when 4 or more weeks of desensitizing toothpaste, fluoride, and bonding have failed on a specific tooth.
Hydroxyapatite-based whitening serums represent a clinically validated approach to simultaneous whitening and sensitivity protection — the mineral fills exposed dentinal tubules while the whitening agent lifts stains, avoiding the permeability spike caused by peroxide-only formulas.
The SNOW Extra Strength Whitening Pen uses this mechanism: apply before and after whitening sessions as a protective buffer for exposed dentin. Backed by over 1,200 five-star reviews (as of 2025).
Get the SNOW Extra Strength Whitening Pen
Final Thoughts
Sensitive teeth pain can feel overwhelming, but it’s usually temporary and treatable. If you need to stop sensitive tooth pain immediately, start with a sensitivity toothpaste, avoid extreme temperatures, and give your teeth a short break from whitening. These simple steps can help soothe sensitive teeth and reduce sharp pain fast.
Long term, protect your tooth enamel by brushing gently, limiting acidic foods, and using products designed for sensitive teeth. At SNOW, we focus on solutions that help minimize tooth sensitivity while still delivering results.
If tooth pain lasts more than two weeks or worsens, see a dentist. Otherwise, with the right care, most sensitive teeth improve quickly.
Frequently Asked Questions (FAQs)
Got more questions? Here are clear, straightforward answers to help you manage sensitive teeth and tooth pain.
How can I stop sensitive teeth pain immediately at home?
Teeth hurt more after whitening because peroxide temporarily increases enamel permeability, leaving the dentin layer's nerve-connected tubules exposed to temperature and acid stimuli. This effect is worse if you already have enamel erosion or early gum recession.
Whitening formulas that include protective ingredients — like the potassium nitrate and nano-hydroxyapatite in SNOW's sensitivity-safe serums — reduce this permeability spike and lower post-treatment pain significantly.
Why does my teeth hurt more after using whitening products?
Teeth hurt more after using whitening products because tooth enamel can become temporarily weakened, and gums may feel irritated. This exposes the inner layer of the tooth, leading to tooth sensitivity and sharp pain with hot or cold foods. It can also be worse if you already have sensitive teeth or early gum disease.
Are natural remedies like clove oil effective for sensitive teeth?
Natural remedies like clove oil can help soothe sensitive teeth by containing compounds that reduce pain and inflammation. Clove oil may offer temporary relief from tooth sensitivity and mild tooth pain. However, it does not treat the root cause, so it’s best used as a short-term solution.
When should I see a dentist for sensitive teeth pain?
You should see a dentist for severe tooth sensitivity if the pain lasts more than 2 weeks or keeps coming back. It’s also important to get checked if you notice swelling, fever, or signs of gum disease. Persistent tooth sensitivity may need professional treatment.
Can switching to a soft-bristled toothbrush help reduce sensitivity?
Switching to a soft-bristled toothbrush can help reduce sensitivity by protecting tooth enamel and preventing gum irritation. Brushing gently lowers the risk of making teeth sensitive or worsening tooth pain. This simple change can help soothe sensitive teeth over time.
How do potassium nitrate and nano-hydroxyapatite work to reduce sensitivity?
Potassium nitrate helps reduce tooth sensitivity by calming the nerves inside the tooth and lowering sharp pain signals. Nano-hydroxyapatite strengthens tooth enamel and repairs tiny surface areas. Together, they help soothe sensitive teeth and provide longer-lasting relief from tooth pain.